1. What influences our health status?
According to a study about the determinants of health status, behavior influeces 40% of the result. This why we have to pay great attention to behavioral risk factors – especially to smoking, consumption of alcohol, unhealthy food and physical inactivity.
Chart 1: Individual behavior greatly influences health results
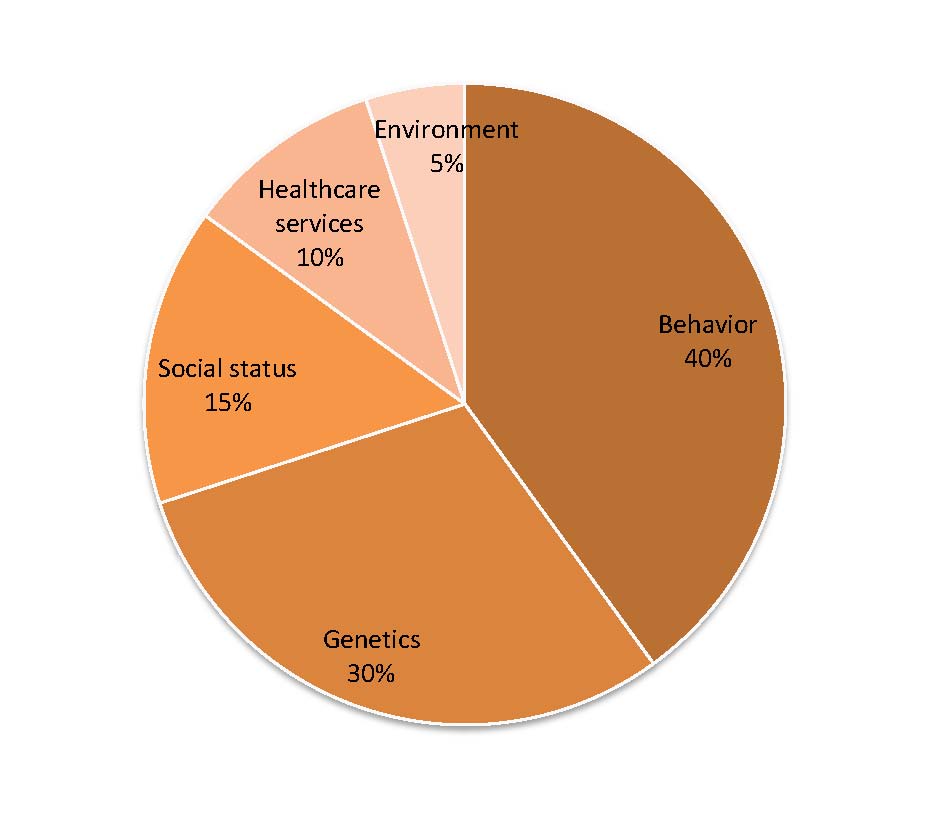
Source: J. Michael McGinnis, Pamela Williams-Russo, and James R. Knickman. The Case For More Active Policy Attention To Health Promotion. Health Affairs, March/April 2002; 21(2): 78-93
2. Behavioral risk factors shorten our lives
People, who moderatly drink alcohol, regurarly practice, stop smoking and eat five times a day fruits and vegetables live, on average, 14 years longer than those, who do not make any of the changes mentioned in their lifestyles.
Table 1: Behavioral risk factors shorten our lives
|
Behavioral risk factors |
Life shortened by |
|
Smoking |
Each smoked cigeratte shortens life by 5 to 7 minutes on average. Life of a smoker is shortened approximately by 8 to 10 years, however, according to some sources this shortage may reach also 13 to 15 years. |
|
Alcohol |
Alcoholics shorten their lives by 23 years. The daily allowed level of alcohol consumption for men is 0.5 to 0.6 liters of beer and 0.25 to 0.3 litres of wine. |
|
Unhealthy food |
At the age of 18, overweight increases the risk of premature death by one third, while obesity doubles this risk. |
|
Physical inactivity |
Even minor physical acitivity, such as 75 minutes of fast walking weakly increases life expectancy by 1.8 years at the age of 40 in comparison to physically inactive people. For instance, fast walking of 450 minutes weakly may contribute to a 4.5 years longer life. |
3. If we know all this, why people do not protect more their health?
The answer has been formulated by Adrian Gore (Republic of South Africa) in 1992, according to whom the problem is with the behavioral economy – the benefits of a healthy lifestyle come at late stages, while costs come very early:
- Maintaining health: costs (time, effort, money) are clear, while benefits are hidden in an uncertain future.
- Healthcare services: Benefits are clear, costs are hidden (due to a reimbursement by a third party.
Therefore, most of the people choose rather consumption of healthcare services than maintaining health.
4. How can we influence behavior of people?
In fact, there are two ways:
- State intervention („top down“ approach) – we may characterize these as restrictive.
- Innovations of the private sector („bottom up“ approach) – we may characterize these as motivating.
5. State intervention for maintaining health
State interventions for maintaining health may be characterized as restrictive. The state tries to influence individual behavior (decreasing the consumption of unhealthy products) threefold:
- Limiting access to certain goods
- Increasing the price of particular goods (According to the study „Price and cigarette consumption in Europe“ from 2005, an increase of real prices of cigarettes by 10% decreases consumption of cigarettes by 5 to 7%)
- Increasing information-sharing of consumers, or not exposing to advertisements
Table 2: Examples of state intervention for particular risk factors
|
Behavioral risk factor |
Limiting access |
Increasing prices |
Increasing information-sharing about possible harms |
|
Smoking |
E.g.: Smoking prohibition in restaurants |
Increasing excise duties on tobacco |
E.g.: Information about the causes on the cigarette packaging
E.g. Prohibition of advertisements for tobacco products |
|
Alcohol |
E.g.: Prohibition of alcohol sales to youngsters
E.g.: Sales only in particular stores |
Increasing excise duties on alcohol |
E.g. Prohibition of advertisements for alcohol before 10pm. |
|
Unhealthy food |
??? I haven’t founds any examples on limiting sales of unhealthy food. I will be glad if you send me one. J |
E.g.: Excise duty for sweetened drinks, or for energy drinks. It is also common that excessive sugar or salt content is being taxed |
E.g.: Obligation to publish nutrition information on the packaging |
|
Physical inactivity |
E.g.: Obligatory sports class at elementary schools |
E.g.: State subsidies for sports education of youngsters or supporting sport fields from public resources |
??? – I haven’t found any state campaign against obesity, I will be happy if you find one and send it to me. J |
6. What are the tendencies in Slovakia?
Some of the interventions are applied in Slovakia. However, efficiency results are not persuasive yet. Here are some of the tendencies between 2003 and 2009 based on OECD data:
- The number of smokers is slightly decreasing
- Alcohol consumption is stable on the level of 10 to 11 liters of pure alcohol per capita
- Number of people with overweight/obesity slightly increases, or slightly decreases (depends on the methodology applied)
Table 3: Smoking, alcohol consumption and overweight/obesity tendencies in Slovakia
|
|
2003 |
2009 |
Tendencies for the past 10 years in Slovakia (according to OECD data) |
|
Smoking population of 15+ population, in % |
22.1% |
19.5% |
Number of smokers slightly decreased |
|
Consumption of pure alcohol in liters yearly (15+ population) |
9.9 (2002: 10.8) |
10.7 (2008: 11.2) |
Alcohol consumption was stable at the level of 10 to 11 liters per capita |
|
% of the population with overweight/obesity according to self evaluation
According to measurements |
47.6%
51.6% (in 2005) |
50.8%
51.5% (in 2008) |
Population with overweight slightly increased, ...
|
Source: OECD, 2013
State interventions seem to be efficient for the reduction of the number of smokers, however, they seem to be less efficient for decreasing the consumption of alcohol or for the fight against overweight/obesity. On the other hand, budgetary effects are very high. In 2012, excise duties on alcohol (spirits, beer and wine) brought approximately EUR 260 million and excise duties on tobacco EUR 635 million. In total, both of these duties made 10.6% of the general budget income in 2012.
7. The private sector is innovating – creation of reward based healthcare (The story of Adrian Gore and his company Discovery Health)
The reaction of the private sector on the current situation was to start dealing with the motivation of people and not with restrictions (as is being done by state interventions). This approach created a new phenomenon „Reward Based Healthcare“, which means healthcare based on rewards. Originally, the approach has been established in South Africa (by the already mentioned Adrian Gore and his company Discovery with the program VITALITY), nowadays, it is however applied practically in each healthcare plans with high individual participation and personal medical accounts in the USA.
The motivation system VITALITY is based on client agreements – focus on what we all (insurance company, doctor and the insured) think is good for you and we give pleasure for you. In the motivation program, there are benefits, which are not distributed automatically, but on the basis of rewards for the desired behavior.
The core of the VITALITY program is that, after filling out a questionnaire, each client receives a so-called Vitality age = biological age, profile of the risk that he/she can affect and a specific wellness plan.
Vitality age works in a way that the risk calculated with a predictive model is expressed as a shortened life expectancy. For instance, the vitality age of a 45 year old man, who is obese, smokes and has high cholesterol level is 59 years.
When meeting a specific wellness plan, the individual receives vitality status: blue, bronze, silver or gold. The acquired status brings benefits for the individual – rewards that may be utilized when maintaining his/her vitality status.
Rewards depend on the vitality status of the client and may include: discounts on sports equipment, fitness, but also for restaurants, discounts on flight tickets, reconditioning visits and vacations.
Sunday Times rewarded Adrian Gore in 2010 as the Business Leader of the Year, in 1998 he was appointed the best businessman in South Africa in a project ran by Ernst & Young reward for the best businessman of the year. Adrian Gore works as an actuary.
8. And the results? (according to the presentation of Adrian Gore)
There is a correlation between the active fulfillment of the “Vitality program” and lower healthcare costs. If such a correlation does exists, is it only thanks to the risk selection or the result of wellness activities? And if it is the result of wellness activities, can the reward based system motivate people to change their behavior?
The answer can be provided by an extensive study for the period 2003 – 2007, which confirmed that an active care for health decreases the costs of health insurance. The influence is the higher the more often the client is being sick!
Members with low activities in the VITALITY program have lower expenses by 21%. Members with greater activities in the VITALITY program have lower expenses by 29%.
9. Summary
- Behavior is responsible for 40% of an individual’s health result.
- Behavioral risk factors (smoking, alcohol, unhealthy food, physical inactivity) may shorten our lives in a great extent.
- Benefits for a healthy lifestyle come at later stages, while the costs come very soon.
- State interventions are mostly restrictive (they ban something), they increase the price of unhealthy goods (through excise duties) or inform about its harmful effects
- The efficiency of state interventions is questionable in relation to improving health status, however excise duties on alcohol and tobacco made more than 10% of the general budget income in 2012
- Motivation of people to maintain their health status is utilized by the concept of „Reward based healthcare“ – it rewards people for taking care for their own health
- Results are very promising – members involved in the program in a greater extent have lower healthcare costs by 29%
The next lecture will be dedicated to the question of, why healthcare cannot be “free of charge”.
Recommended bibliography
1. J. Michael McGinnis, Pamela Williams-Russo, and James R. Knickman. The Case For More Active Policy Attention To Health Promotion. Health Affairs, March/April 2002; 21(2): 78-93
2. Price and cigarette consumption in Europe, 2005
3. OECD Health Data, 2013
4. Údaje z prezentácie Adriana Gore-a (s láskavým dovolením Tomáša Macháčka)









Comments
2 comment(s). Display all comments.
znie to pekne ale je to inak somarina, stat sa snazi donutit ludi zaujimat sa o svoje zdravie a robi to tak ze zdrazuje formou vyzsej sadzby dane urcite vyrobky, otazka je co s peniazmi co vyzbiera ci aj investuje s5 do neefektivneho zdravotnictva. Pan Adrien Gore ne-objavil koleso :( je logicke ze ak sa clovek o svoje zdravie zaujima a stara stoji to menej kedze neni tolko chory. Otazka znie, komu uspori peniaze. Jemu odvody neklesnu, akurat uspori poistovni. Keby p. gore radsej tlacil na to aby sa odvody za zdravototnu starosltivost neplatili a ludia si za tie peniaze mohli zaplatit zdravotnu starostlivost sami. Poistovne by boli nutene nahanat klientov, aby zarobili, teraz to robit nemusia. Ak by sa klient o seba staral co je cielom statu, poistovna by mu mohla zlacnit poistne (aby mohla konkurovat inej poistovni) lenze… co robi stat… to stoji za ...
Dobry den, prikladom statnej regulacie dostupnosti nezdravych potravin by mohli byt: zakaz predaja nezdravych potravin na skolach (Lotyssko, Rumunsko), alebo zakaz reklamy na nezdrave potraviny v programoch pre deti (Velka Britania). Za nezdrave potraviny povazuju napriklad tie, ktore maju velky obsah cukru alebo obsahuju niektore farbiva.